Pancreatic cancer still has a high mortality despite advances in cancer treatment. The drug of choice for the clinical treatment of pancreatic cancer is gemcitabine. Bacteria present in pancreatic cancer tissues can degrade gemcitabine to 2,2′-difluorodeoxyuridine nucleoside (dFdU), which is inactive, leading to drug resistance.
Traditional antibiotics are not well-suited for the effective treatment of pancreatic cancer due to the lack of tissue selectivity. Bacteria in the tumor (intratumoral bacteria) are killed along with gut bacteria. The development of new antimicrobial treatments that selectively target the bacteria in pancreatic cancer tissues could be useful for overcoming drug resistance and improving the therapy of pancreatic cancer.
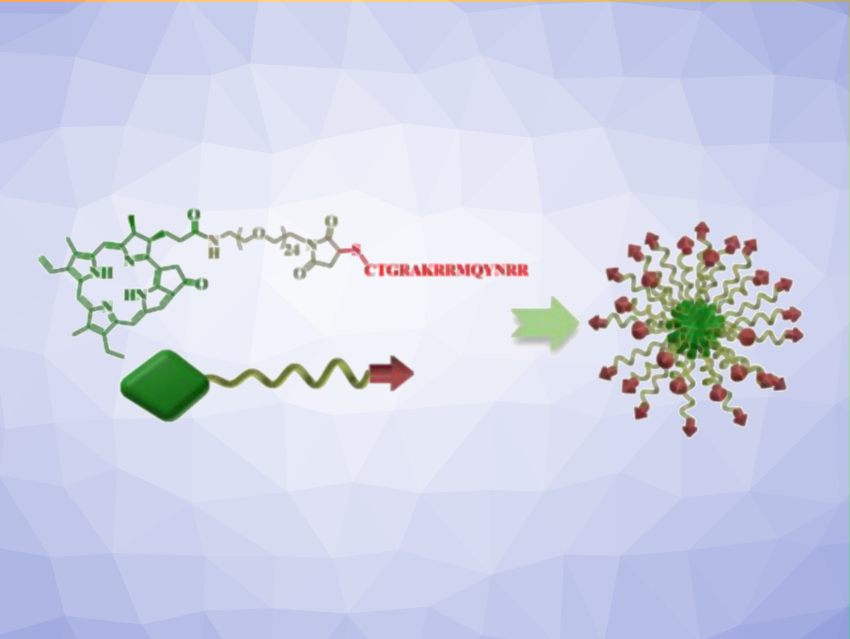
Renfa Liu, Yunxue Xu, Zhifei Dai, Peking University, Beijing, China, Linxue Qian, Capital Medical University, Beijing, China, and colleagues have developed an antibacterial photodynamic therapy to selectively eradicate intratumoral bacteria. An antimicrobial peptide was linked to a chlorophyll-derived photosensitizer through a poly(ethylene glycol) chain. The resulting structure can self-assemble into micelles with a diameter of about 20 nm (pictured). The peptide endows the micelles with bacteria-targeting capabilities.
The micelles can efficiently kill bacteria under near-infrared (NIR) light irradiation by inducing membrane damage, thereby inhibiting the conversion of gemcitabine. In an animal model of pancreatic cancer, the selective photodynamic eradication of intratumoral bacteria efficiently reversed gemcitabine resistance. This work shows that antibacterial photodynamic therapy could be a promising strategy for improving cancer therapy by changing intratumoral bacterial communities.
- Photodynamic eradication of intratumoral microbiota with bacteria‐targeted micelles overcomes gemcitabine resistance of pancreatic cancer,
Renfa Liu, Huanyu Yang, Shuai Qu, Peipei Yang, Xin Zhi, Yunxue Xu, Zhifei Dai, Linxue Qian,
Aggregate 2023.
https://doi.org/10.1002/agt2.423